Eye Library / Diagnostic Tests / Tonometry
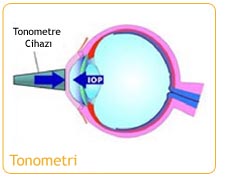
Tonometry is used to measure the intraocular pressure (IOP) by recording the resistance of your cornea to pressure. It is used to screen for glaucoma. There are different tonometry methods.
Applanation (Goldmann) Tonometry uses a small probe to gently flatten part of your cornea to measure eye pressure and a microscope called a slit lamp to look at your eye. The pressure in your eye is measured by how much force is needed to flatten your cornea. A strip of paper containing a dye (fluorescein) will be touched to your eye. The dye makes it easier for doctor to see the cornea. This type of tonometry is very accurate.
Indentation (Schiotz) Tonometry uses a plunger to gently push on your cornea. The pressure in your eye is measured by how much weight is needed to flatten your cornea. This test is not as accurate as applanation tonometry and is not used very much. However, some family medicine doctors or urgent care doctors may still commonly use this test.
Noncontact Tonometry (pneumotonometry) does not touch your eye but uses a puff of air to flatten your cornea. This type of tonometry is not the best way to measure intraocular pressure. But it is often used as a simple way to check for high IOP and is the easiest way to test children. Noncontact tonometry does not use numbing eyedrops. The patient rests his/her chin on a padded support and stares straight. A brief puff of air is blown at the eye. Patient hears the puffing sound and feels a coolness or mild pressure on his/her eye. The tonometer records the intraocular pressure (IOP) from the change in the light reflected off the cornea as it is indented by the air puff. The test may be done several times for each eye.
It is a good idea to have the intraocular pressure checked routinely after the age of 40, or if you are at a high risk for developing glaucoma.





