Eye Lid Inflammation
Eyelids consist of thin folds of skin, muscle, and connective tissue. They protect the eyes and spread tears over the front of the eyes. The inside of the eyelids are lined with the conjunctiva which is called the palpebral conjunctiva. The outside of the lids are covered with the body's thinnest skin.
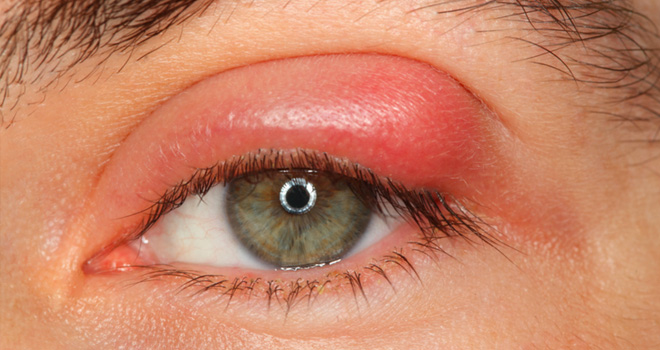
Eye lid inflammations include mainly stye, blepharitis, chalazion. A stye is an infection of one of the three types of eyelid glands near the lid margins, at the base of the lashes. A chalazion is an enlargement of a meibomian gland which is an oil-producing gland in the eyelid. This is usually not associated with an infectious agent. More likely, the gland opening is clogged. Initially, a chalazion may resemble a stye, but it usually grows larger. A chalazion may also be located in the middle of the lid and be internal.
Blepharitis is the inflammation of the eyelid margins, often with scales and crust. It can lead to eyelash loss, ectropion, corneal damage, excessive tearing, and chronic conjunctivitis.. Incidence of eye lid inflammation is 1.8 per 1000 per year. It accounts for 4.5% of all ophthalmological problems.
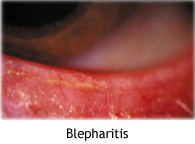
The inflammation of the eyelid margins often results with scales and crust. It can lead to eyelash loss, ectropion, corneal damage, excessive tearing, and chronic conjunctivitis.
If these eyelid disorders are not treated, they can lead to other, possibly serious vision problems-dry eye, astigmatism, or even vision loss. An ophthalmologist or optometrist should be consulted. Good lid hygiene is very important. Regular eyelid washing with baby shampoo or special lid scrub helps prevent styes, chalazia, blepharitis, and eyelid edema. To avoid these problems, it's also important to refrain from touching and rubbing the eyes and eyelids, especially with hands that have not just been washed.
Eye lid inflammation is mainly caused by bacterial infection or allergies.. With the most common seborrheic form, dry, flaky patches of skin may develop. Dandruff is common on the scalp and the eyebrows.
Sore eyes that are burning and gritty with crusting on waking - usually bilateral and chronic. The eye(s) may be red and occasionally, patients complain of epiphora (tearing) or dry eye and photophobia.
There are a number of signs, some characteristic to each type of blepharitis and many overlapping where there is mixed pathology
Styes are usually caused by bacterial staphylococcal infections. The symptoms are pain and inflammation in one or more localized regions near the eyelid margin.
A chalazion is caused by a blockage in the outflow duct of a meibomian gland. Symptoms are inflammation and swelling in the form of a round lump in the lid that may be painful.
Some cases of blepharitis are caused by bacterial infection , but in some cases, the cause is unclear. It may also be caused by an overproduction of oil by the meibomian glands. Blepharitis can be a chronic condition that begins in early childhood and can last throughout life. Symptoms can include itching, burning, a feeling that something is in the eye, inflammation, and scales or matted, hard crusts surrounding the eyelashes.
Blepharitis usually causes symptoms of eye itching, burning, and soreness. Vision is usually normal, although a poor tear film often blurs vision. Redness, warmth, and swelling may also be noted. Eyelid matting or "gluing" of the lashes are common. Some forms result in yellow- or green-colored infectious discharge.

An ophthalmologist usually diagnoses this condition after a careful history and an examination of your eyes and eyelids.
Some diseases may affect your eyes, so some of the questions or the examination may be focused on other parts of your body.
The cornerstone of therapy is good eyelid hygiene.
Styes are treated with warm compresses for 10-15 minutes, three to four times a day. Sometimes topical antibiotics may be prescribed if the infection is spreading. You may be prescribed a topical antibiotic if your ophthalmologist believes that you have an infectious form of blepharitis. Occasional blurriness may occur after eyedrops or ointments are placed in your eyes. This should clear up quickly.
One fourth of chalazia will disappear spontaneously, but warm compresses may speed the process. Chloramphenicol ointment may be used as well. Because chalazia are inside the lid, topical medications are generally of no benefit. Medication may need to be injected by the doctor into the chalazion or if that doesn't help the chalazion may need to be excised. If what appears to be a chalazion recurs on the same site as any previous one, the possibility of sebaceous gland malignancy should be investigated by biopsy.
Blepharitis is treated with hot compresses, with antibiotic ointment, and by cleaning the eyelids with a moist washcloth and then with baby shampoo. Good hygiene is essential. Patients can try to keep rooms dry, such as by placing a bowl of water on top of a radiator. Tear film supplements can help moisten the eyes when dry. If itching, soreness, or redness occurs from the tear film drops, they should be stopped. Topical or systemic antibiotics also may be prescribed. If the blepharitis doesn't clear up with treatment or if it seems to be a chronic problem, the patient may have acne rosacea. These patients may need to see a dermatologist as well.
Last Updated: October 23, 2024